By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
The annual AAO-HNSF International Tinnitus Mini-Seminar convened in Washington, DC on September 10, 2012. It was held in conjunction with the annual meeting of the American Academy of Otolaryngology – Head and Neck Surgery Foundation (AAO-HNSF). The subject of the seminar was Radiology and Brain Imaging Techniques.
This seminar was previously known as the International Tinnitus Forum, which was held during the same time frame but not under the auspices of the AAO-HSNF. Now it is a foundation seminar that provides Continuing Medical Education (CME) credits for physicians to use in furthering their knowledge.
The content of this seminar was extremely technical, using PowerPoint presentations including many brain scan images. It is not possible to convey all the information contained in the presentations. I will try to provide an overview of what was discussed in general terms.
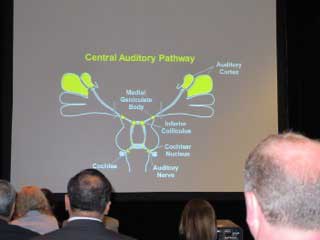
Jennifer Melcher, MD presented on functional Magnetic Resonance Imaging (fMRI) studies and their findings on people with tinnitus. One study was imaging of the central auditory pathway from the auditory nerve to the auditory cortex.
She studied people who have tinnitus but normal hearing thresholds and compared them to patients who do not have tinnitus. Both groups, therefore, have normal hearing but one group has tinnitus while the other does not.
Tinnitus patients had elevated response to sound and hyperactivity in the brainstem even though both groups had closely matched hearing thresholds. There are other areas of the brain, beside the auditory cortex, which influence the perception of tinnitus. This may lead to a deeper understanding of the neurological and cognitive/emotional aspects of tinnitus.
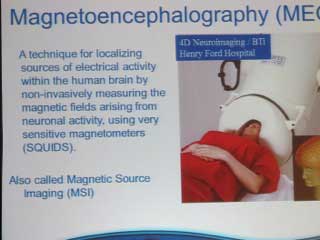
Susan Bowyer, PhD discussed Magnetoencephalography (MEG) imaging. This is a way of localizing electrical activity within the brain by measuring the magnetic fields caused by neuronal activity. It is extremely sensitive and can measure changes in milliseconds.
The technology became available in the 1980’s but with a limited number of sensors so brain scanning had to be done in segments. In the late 1990’s, the technology was evolved enough to conduct whole head scanning.
Dr. Bowyer has been working with Dr. Michael Seidman for several years using MEG technology to study tinnitus patients. They map the brains of people listening to their own tinnitus for 10 minutes, then give them tones at 1,000 Hz followed by pitch-matched tones of their tinnitus.
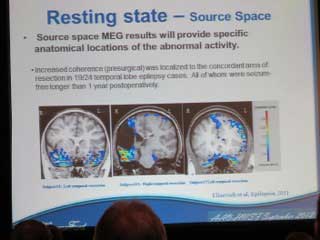
Dr. Bowyer works in the Neurology Lab at Henry Ford Health System and her studies also involve epilepsy patients. They have been able to localize epileptic networks in the brain that have been hyperactive and use this information to remove the tissue. They have looked at patients who are 1-2 years post-operative and are seizure free. The surgeries were performed using MEG imaging to point where the problem areas were located. The same neuronavigation technique can be used to localize hyperactive networks in tinnitus patients’ brains.
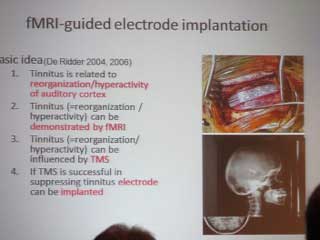
Dirk de Ridder, MD discussed imaging techniques that can be used to neuronavigate the brain to guide in implanting electrodes to attempt to control tinnitus. Dr. de Ridder has worked with Dr. Michael Seidman in this area.
One of the most common causes of tinnitus is a lack of input due to hearing loss. Less information arrives at the level of the thalamus and it starts to slow down. The slowing down of the specific area that lacks input causes a decrease in lateral inhibition and there will be a halo around the area of high frequency gamma band hyperactivity. The intensity of the gamma activity may be related to the loudness of the tinnitus.
Either fMRI or MEG can be used to locate areas in the auditory cortex with tinnitus. These areas can be targeted using non-invasive Transcranial Magnetic Stimulation (TMS). TMS causes an electrical field to be generated inside the brain in the area of the hyperactivity. There has been a lot of research into the use and efficacy of TMS recently.
If the TMS is successful in dampening the tinnitus, the next step can be taken for people with debilitating tinnitus. This involves the implanting of an electrode array in the area of the auditory cortex that is causing the problem. The array will have several electrodes along its length. These electrodes can be turned on and off experimentally until maximum tinnitus suppression is reached.
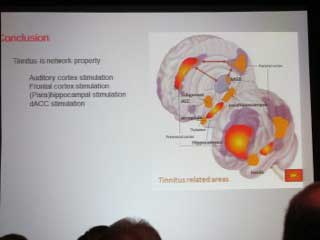
The discussion continued by looking at other areas of the brain that influence tinnitus and where additional electrode arrays may be helpful. Tinnitus is a network phenomenon and not simply located in the auditory cortex. These are very preliminary ideas and much more work needs to be conducted to define the treatments better.
Arnold Strashun MD discussed central debilitating tinnitus and nuclear medicine. Nuclear medicine imaging techniques include SPECT (single photon emission computed tomography) and PET (positron emission tomography). These imaging techniques employ gamma rays to provide a true 3-D image of the brain. These images can be manipulated by the computer and typically allow the viewer to view thin slices of the brain.
Blood flow studies can be conducted showing how the brain uses oxygen and glucose, the two fuels for brain operation. This shows metabolic activity in areas of the brain and can isolate areas of hyperactivity.
The discussion continued to the neuronal networks that affect tinnitus. It is not only the auditory cortex, but elements of other brain structures are involved in a neuronal loop.
Dr. Strashun used a pharmacologic agent that locks onto GABA receptors, the primary inhibitive neurotransmitter in the brain. The GABA receptor has been identified by Dr. Abraham Shulman as the central pathway through the brain through which all tinnitus signals must travel.