By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
Hyperbaric Oxygen (HBO) has long been used as the primary treatment for divers who suffer from decompression sickness and people with carbon monoxide poisoning. It is an adjunct treatment for 14 other conditions including radiation damage, crush injuries, skin grafts and burns. Medical coverage for treating diabetic ulcers began in 2003. Now there is significant medical evidence supporting its use for Sudden Sensorineural Hearing Loss and tinnitus, at least in the early stages. Here is the story.
In the first documented use of hyperbaric therapy, a British physician used compressed air for medical purposes in 1662 and elemental oxygen was discovered in 1775. HBO therapy for treating diving accidents was proposed in 1917 but it was not until 1937 that the first true HBO therapy was used for decompression sickness.
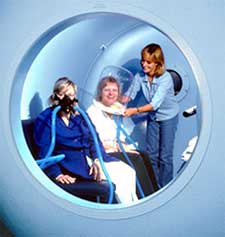 During hyperbaric oxygen therapy (HBOT) the patient sits inside a pressurized chamber. These chambers have been designed to hold one or multiple individuals. Air pressure inside the chamber is increased up to 2.5 times normal atmospheric pressure at sea level.
During hyperbaric oxygen therapy (HBOT) the patient sits inside a pressurized chamber. These chambers have been designed to hold one or multiple individuals. Air pressure inside the chamber is increased up to 2.5 times normal atmospheric pressure at sea level.
The patient then breathes pure oxygen from a mask. The air inside the chamber is of normal composition at all times. Typical HBOT sessions last for 1 or 2 hours and are repeated 10 or 15 times on successive days. In the chamber patients can read, watch movies or converse with others.
There are no adverse side-effects to HBOT. Occasionally a patient complains of claustrophobia. When this is suspected, clinicians will usually allow the person to slowly adjust to being in the chamber for a few minutes at a time until the problem is reduced to manageable proportions. Occasionally anti-anxiety medications are used.
Due to the increased pressure inside the chamber, far more oxygen is dissolved in the bloodstream than under normal conditions. HBOT enables the oxygen content of the blood to reach up to 7%, which is 20 times higher than normal. Those parts of the body which suffered damage due to poorly supplied oxygen are now exposed to significant quantities. This allows biological processes which are dependent on oxygen to be initiated. In 40% of cases, improvement in the patient’s condition continues even after treatment has stopped.
HBOT increases oxygen pressure in the inner ear. Oxygen flows from areas of higher pressure to those of lower pressure. It has been shown there is a profound decrease in oxygenation of the cochlea during and after acoustic stress and in acute hearing loss. During exposure to HBOT the oxygenation in the cochlea increases up to 460% and is still 60% above normal one hour after termination of the therapy.1
With an increase of the pressure of oxygen in the cochlea, it is possible to influence the sensory cells of the inner ear. These cells have no direct vascular supply and depend entirely on oxygen supplied by diffusion. An increase in oxygen pressure can compensate for oxygen deficiency caused by trauma and gives rise to biological mechanisms that are involved in functional recovery.
Hair cells in the inner ear react in a uniform way to damage, whether caused by noise, viruses, ototoxic substances (those which are toxic to the ear) or hypoxia (oxygen deficiency). The hair cells first swell and lose their function. This effect is reversible in cases of minor damage and sometimes hair cells with minor damage will regain function. In cases of severe damage or if the swelling persists for more than one year, the hair cells degenerate completely and are replaced by non-functioning cells.
Accordingly, most of the studies show that HBOT is most effective in reducing hearing loss and tinnitus in the first three months following hearing loss or acoustic trauma. Regarding hearing loss alone, an overview of clinical studies from Germany shows HBOT is effective in 50% of cases in reducing hearing loss by 20 dB or more. Approximately 11% have a full recovery.
Regarding tinnitus, evaluations of 7766 patients in the same overview showed reduction of the intensity of tinnitus by 50% in approximately 70% of the cases treated within 3 months. Approximately 30% of patients had their tinnitus completely resolved. Tinnitus with duration of more than 3 months showed a 50% improvement in the intensity of tinnitus in 30% of patients. After 12 months of chronic tinnitus, no improvement was seen.2
Another study, conducted in Europe but published in the US, studied 50 patients who were admitted within 48 hours of sudden hearing loss. This study did not rate severity of tinnitus but degree of hearing loss. Thirty patients underwent HBOT while 20 were given vasodilators. Of the 30 HBOT patients, 25 (83.3%) experienced either a very good (50% or more) or a significant (25% to 50%) improvement.3
Despite the stipulation that the best treatment results are seen in early onset cases, many people in Germany and Europe with chronic tinnitus and hearing loss are treated with HBO. In Germany there are approximately 80 multi-person hyperbaric oxygen chambers and 80% of the treatments are for inner ear dysfunction. The German Society for ENT Diseases refers to HBOT as one among other accepted treatments for symptoms of hearing loss, tinnitus, vertigo, head injury and trauma. Six new controlled studies on HBOT are currently being conducted in the country. German health insurance covers the cost of the treatments in most cases.
In the United States, many health insurance providers, including MediCare, provide insurance coverage in cases of sudden deafness or noise-induced hearing loss provided treatment is initiated within 3 month of onset. However, no coverage for tinnitus (recent onset or otherwise) is provided. The cost of a single session in the US is between $300 and $400.
HBO chambers can be found in private clinics and in many hospitals throughout the United States and Europe.
Footnotes
1. Lamm K.; Simultane Sauerstoffpartialdruckestimmung in der Skala Tympani, Electrokochleographie und Blutdruckmessungen nach Knalltraumata bei Meerschweinchen. HNO 37(1989)48-55.
2. Lamm H.; Deer Influx deer hyperborean Sauerstofftherapie auf den Tinnitus und den Horverlust bei akuten und chronischen Innenohrschaden. Otolaryngol Nova 5 (1995) 161-9.
3. Fattori B, Berrettini S, Casani A, Nacci A, De Vito A, De Iaco G. Sudden Hypoacusis treated with hyperbaric oxygen therapy: a controlled study. Ear, Nose & Throat Journal Sept. 2001.
