By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
Someone recently told me he had been diagnosed with iron deficiency, and after he began iron supplement therapy, his long-standing tinnitus was dramatically improved. I went looking and discovered a couple of studies showing that iron deficiency can cause hearing loss and tinnitus. Later, after digging a little deeper, I learned that it can worsen hypothyroidism too.
Iron Deficiency and Tinnitus Relief
One study, conducted in China and published in PubMed, found iron deficiency (also called iron anemia) in 61% of those with sudden hearing loss. (1)
The second study, published in Otolaryngology, Head Neck Surgery, showed a direct association between sudden hearing loss and iron deficiency. It was most pronounced among subjects 44 years or younger, but also affected those up to 60 years old. (2)
This is especially relevant because over 80% of people with tinnitus have it due, at least in part, to hearing loss.
The University of Maryland website lists tinnitus as a common side effect of iron deficiency or anemia. (3)
Finally, another report calls pulsatile tinnitus a common symptom of anemia. Anemia causes low blood viscosity, which increases blood flow. Anything that increases blood flow can cause pulsatile tinnitus. (4)
In those with tinnitus and iron deficiency or anemia, iron supplements can reduce the loudness and aggravation of tinnitus and provide tinnitus relief.
Iron Deficiency and Hypothyroid Relief
Iron anemia is often found in those with hypothyroidism, which studies identify as a possible cause of anemia. One study found anemia present in 43% of overt hypothyroid patients and 39% of subclinical hypothyroid patients. (5)
A paper from Dr. Nikolas Hedberg describes how low iron levels have been the missing link in some patients with hypothyroidism who can’t balance their thyroid levels and still have symptoms after thyroid hormone treatment. Supplementing with iron helped reduce hypothyroid symptoms, including tinnitus. (6)
Dr. Westin Childs calls iron deficiency one of the most common nutrient deficiencies in hypothyroid patients, even if they are currently taking thyroid medication. The connections are clear. Not only is iron required for the creation of thyroid hormone, but low iron levels are also associated with low levels of free T3, the active form of thyroid hormone. Patients with hypothyroid should have their iron levels checked; most health providers only check iron levels if they find grossly abnormal hemoglobin or red blood cell levels. (7)
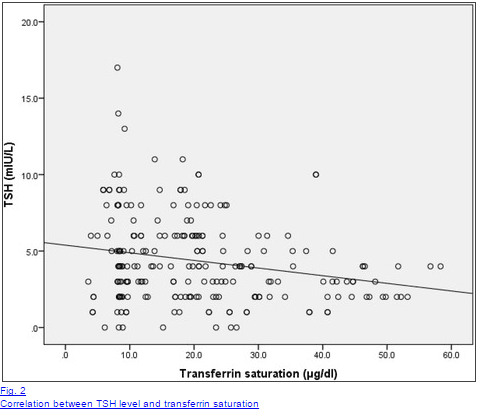
The accompanying chart shows the relationship between iron (ferritin) saturation and TSH levels. As iron saturation falls, TSH increases, indicating hypothyroidism.
In the typical person with an under-active thyroid gland, the blood level of T4 (the main thyroid hormone) will be low, while the TSH level will be high. This means that the thyroid is not making enough hormone, and the pituitary recognizes it and is responding appropriately by making more Thyroid Stimulating Hormone (TSH) in an attempt to force the thyroid to produce more.
How Iron Affects the Body
Iron is a key part of various proteins and enzymes. It is responsible for the transport of oxygen and the regulation of cell growth, among many other functions.
One of its most important roles is in hemoglobin, a component of red blood cells which binds to oxygen and carries it throughout the body. Without proper oxygenation, cells begin to die.
Too little iron leads to problems such as:
- Fatigue
- Profound exhaustion
- Decreased immunity
- Weakness
- Dizziness
- Tinnitus
- Memory loss
- Leg and chest pain
- Many other symptoms
Iron overload can be dangerous too, and is a far more common problem than iron deficiency, especially in men.
Too much iron leads to problems such as:
- Brain fog
- Fatigue
- Low sex drive
- Mood swings, especially anger
- Digestive problems
- Anxiety
- Depression
- Other symptoms
Men, Women, and Iron Deficiency
Small amounts of iron are lost in urine, feces, and dead skin cells. Far larger amounts are lost through bleeding. This is why premenopausal women are most at risk of becoming iron deficient. Even postmenopausal women can be iron deficient, if they developed a large deficiency previously and have not built iron stores back up to normal. Iron deficiency can also result from internal bleeding, such as from cancer or an ulcer.
Because the biggest source of iron is meat, vegetarians and vegans are also more likely to develop iron deficiency. They must be careful to get enough iron from other sources, such as tuna and other oily fish, beans, tofu, eggs, wholegrain breads, green vegetables and dried fruits.
Taking Vitamin C with meals helps the body absorb more iron.
For those who have iron overload, certain herbs and spices, such as green tea and rosemary, can reduce iron absorption. The polyphenol curcumin, found in turmeric, acts as an iron chelator and helps remove iron from the body.
Blood Tests for Iron Deficiency and Overload
There is a simple blood test for iron levels, the serum ferritin test. The test measures ferritin, the carrier molecule of iron. If ferritin levels are low, iron levels are also low.
The healthy range of ferritin lies between 20 and 80 ng/ml (nanograms per milliliter). The ideal range is between 40-60 ng/ml.
People who have unresolved hypothyroidism or chronic tinnitus should have their ferritin levels checked to rule out iron deficiency.
References:
1 –https://www.ncbi.nlm.nih.gov/pubmed/9812800
2 – Chung SD, Chen PY Lin HC, Hung SH. Sudden sensorineural hearing loss associated with iron deficiency anemia. JAMA Otoleryngol Head Neck Surg. 2014 May; 140(5):417-22.
3 – http://www.umm.edu/health/medical/reports/articles/anemia
4 – http://www.tinnitushearingsolutions.com/medicalsolutions/medical-causes-of-tinnitus/anaemia-and-tinnitus/
5 – Erdogan M, Koseni A, Ganidagli S, Kulaksizoglu M. Characteristics of anemia in subclinical and overt hypothyroid patients. Endocr J. 2012:59(3):213-20.
6 – https://drhefberg.com/theferritintest
7 – https://www.restartmed.com/hypothyroidism-iron-deficiency/
Get Free Shipping!
Order now and get free shipping on either the Tinnitus Starter Kit or Combo Pack. Try the doctor recommended products with clinically proven ingredients for tinnitus. No coupon code required.

