Risk Factors for Hearing Loss & Tinnitus
By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
The American Tinnitus Association reports that up to 90% of all people with tinnitus have some level of hearing loss.Now, further evidence on the relationship between poor health and hearing loss has been published in a recent article in Otology & Neurotology.1
The objective of this important study was to evaluate and compare the effects of cardiovascular risk factors (hypertension, smoking and diabetes), noise exposure (occupational, recreational and firearm), and the synergistic interactions between them on frequency-specific hearing thresholds.
The study was based on results from the National Health and Nutrition Examination Survey (NHANES). This is an ongoing survey of the civilian, non-institutionalized population of the US which occurs every two years. In the 2000 and 2002 survey, NHANES collected sample audiometric data on 3,853 US adults aged 20 to 69 years which was used in the study.
Audiometry was performed using a mobile examination center. Hearing thresholds were determined for each ear from 0.5 to 8 kHz. Interviewers administered detailed questionnaires which included age, sex, education, ethnicity, exposure to recreational or occupational noise, including gunfire, power tools and loud music. A complete smoking history was compiled including the number or years smoked and the current number of cigarettes smoked per day. A history of hypertension and diabetes was also recorded.
The percentages of risk factors in the study population were as follows:
| Heavy smoking |
16%
|
| Hypertension |
27%
|
| Diabetes |
7%
|
| Occupational noise exposure |
33%
|
| Recreational noise exposure |
25%
|
Heavy smoking and a history of diabetes were associated with significantly increased odds of hearing loss as was occupational and firearm noise. There were not any significant differences based on age, sex, ethnicity or educational level.
Associations between cardiovascular risk, noise exposure and hearing levels at specific frequencies were also analyzed. People with diabetes had significantly worse hearing levels at low (1 kHz) and high (3-8 kHz) frequencies compared to people with no diabetes. Heavy smokers also had significantly worse hearing levels and both low and high frequencies. Participants with hypertension had diminished hearing levels at 1 kHz only.
(Fig. 1)
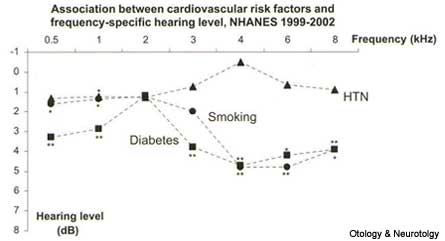 FIG. 1 – HTN = Hypertension
FIG. 1 – HTN = Hypertension
The pattern of frequency-specific hearing loss associated with cardiovascular risk was compared to the pattern observed with noise exposure. Participants with firearm noise exposure had significantly poorer hearing levels compared to those without firearm exposure, particularly at high frequencies (4, 6, and 8 kHz). (Fig. 2)
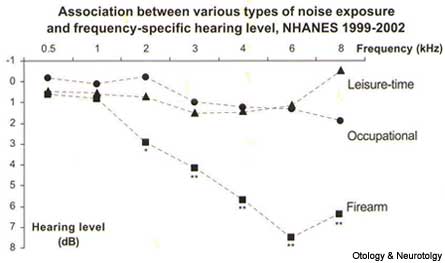 FIG. 2
FIG. 2
Combined exposure to smoking, cardiovascular risks and noise exposure were evaluated to see if there was a greater-than-additive influence on the odds of frequency-specific hearing loss. It was found that differences in hearing levels among those with and without firearm noise were greater among heavy smokers than nonsmokers. For example, at 8 kHz, firearm noise was associated with an 8 dB reduction in hearing among heavy smokers compared with a 2 dB reduction among nonsmokers. (Fig. 3)
There was also observed significant interactions between firearm noise exposure and diabetes at 3 kHz (Data not shown).
Metabolic vs Sensory Hearing Loss
This study found that both smoking and diabetes increased the odds of hearing loss twofold. Both were significantly associated with hearing loss across the frequency spectrum. In contrast, noise exposure was significantly associated with hearing loss in the high frequencies.
These two distinct patterns of hearing loss mirror what is often termed “metabolic” and “sensory” hearing loss. Metabolic hearing loss refers to pathology of microvascular (capillary) origin that affects the entire cochlea. Agents of microvascular disease (smoking and diabetes) produce a broad spectrum pattern that shows up as a relatively flat audiogram (hearing loss across the frequency spectrum).
Sensory hearing loss is associated with noise exposure and a down sloping audiogram. This study found that heavy smokers were significantly more likely to incur hearing loss from firearms compared to nonsmokers. Several studies suggest that noise exposure leads to the formation of reactive oxygen species, or “free radicals”, with the capacity to produce hair cell death in the cochlea. Microvascular disease may impair the delivery of antioxidant molecules and limit an individual’s ability to recover from noise trauma. This is reinforced by the recent findings that antioxidant supplementation significantly reduced hearing loss if taken shortly after noise exposure.
Conclusions
These findings suggest that smokers and people with diabetes are particularly at risk for hearing loss and may benefit from hearing loss screening in much the same way as people with diabetes are currently screened for retinopathy. Smokers and people with diabetes should be counseled to embrace lifestyle modifications and to avoid excessive noise exposure to reduce the risks associated with the synergistic effects between these toxicities.
Reference:
1- Agrawal Y, Platz EA, Niparko, JK. Risk Factors for Hearing Loss in US Adults: Data from the National Health and Nutrition Examination Survey, 1999 to 2002. Otology & Neurotology 2009; 30(2):139-145
Get Free Shipping!
Order now and get free shipping on either the Tinnitus Starter Kit or Combo Pack. Try the doctor recommended products with clinically proven ingredients for tinnitus. No coupon code required.


