By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
The “Invisible” Hearing Aid
Rapid progress continues to be made in the field of hearing aid technology. Once clunky, intrusive and unsightly, hearing aids have been miniaturized and digitized for improved performance. Nonetheless, many people are uncomfortable using hearing aids while others do not achieve the promised benefit. Now there is a surgically implantable hearing aid that is totally invisible and provides much better full-frequency audiological response. It also holds out hope for improvement in high frequency tinnitus for many people.
The new hearing aid is named the Esteem from Envoy Medical, commonly referred to as the Envoy Esteem. The device consists of a sound processor with battery connected to a sensor and a driver. The sound processor is implanted under the skin, in the mastoid bone behind the ear, during a surgical procedure that takes about 5 hours.
It must be mentioned at this point that the Envoy Esteem is not a cochlear implant, nor is it intended to compete with them. A cochlear implant is for people with complete deafness and it replaces the cochlea. The Esteem implant is a hearing aid for those with poor hearing.
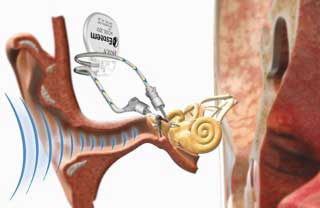
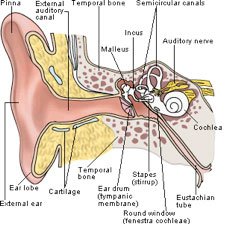 The sensor and driver of the Esteem are connected to two of the three bones of the middle ear that are collectively called the ossicles. These bones are the smallest bones in the human body. They are responsible for transmitting sound vibrations from the eardrum to the inner ear where the vibrations are converted into electrical signals and sent to the brain.
The sensor and driver of the Esteem are connected to two of the three bones of the middle ear that are collectively called the ossicles. These bones are the smallest bones in the human body. They are responsible for transmitting sound vibrations from the eardrum to the inner ear where the vibrations are converted into electrical signals and sent to the brain.
The sensor is connected to the incus bone in the middle ear by means of bone cement. The incus picks up sound vibrations from the eardrum through the malleus bone. This is one of the revolutionary insights that makes this device so unique; it does not require the use of a microphone but instead uses the body’s own microphone, the eardrum, to produce the vibrations.
The signal goes to the sound processor, where it is amplified, and then to the driver. The driver is connected to the stapes bone where it delivers the amplified signal. The stapes bone is attached directly to the round window, the barrier to the inner ear. The signal is then transferred to the cochlea. Essentially the device uses the patient’s own eardrum, bones and nerves but intercepts and amplifies the signal.
There are many obvious advantages to a hearing aid implanted inside the head. For one, it is discrete and no one has to know it is there. There is considerable social stigma for some people about wearing a visible hearing aid in public.
Another advantage is the hearing aid does not have to be protected from water. The person wearing it can shower normally and swim without fear of damaging the device.
Because the batteries are internal to the device, there are no wires running to it and a small remote controller can control it. It can be turned on and off and the amount of amplification can also be controlled. The batteries have to be replaced every four to seven years but that is accomplished in a simple outpatient procedure.
The surgery is so delicate that there are only a handful of doctors in the US who are capable of performing it. Tinnitus authority, Michael Seidman, MD is one of these and has performed several implants. Dr. Seidman is the Director of Otologic Surgery at Henry Ford Hospital in West Bloomfield, MI.
If the tiny metal parts are not cemented to the bones in perfect position, the device won’t work properly. “We have a clinical field engineer mandated by the FDA in every single procedure, and after we perform the main steps, they can verify that this is indeed going to work before we wake the patient up,” stated Dr. Seidman. He describes this as “the ultimate in microsurgery.”
The device is turned on for the first time 8 weeks after surgery. Turning it on earlier than 8 weeks usually results in feedback and distortion that can be very annoying for the patient. The cause is fluid in the mastoid under the implant caused by the surgery. The body absorbs this fluid after 8 weeks.
A clinical trial was conducted between January 2008 and August 2009 on 57 subjects.1 Speech recognition thresholds improved from baseline hearing aid assisted (BLA) of 41.2 dB hearing loss down to 29.4 dB with the Esteem. Word recognition score at 50 dB improved from BLA of 46.3% to 68.9% with the Esteem.
The authors concluded, “Phase 2 results at 12 months post implant demonstrated that (1) hearing results with the device are statistically superior to baseline best-fit hearing aids for speech recognition thresholds and word recognition score and (2) the device is safe.
A separate paper based on the same study separated out five patients who were identified with profound, high frequency sensorineural hearing loss.2 This is the hearing loss range that causes most cases of tinnitus. The study used three different testing conditions: Baseline unaided (no hearing aid) referred to as BLU, Baseline hearing aid assisted (BLA) and 12 month postoperative Esteem.
The study showed the Esteem provided greater amplification in the higher frequencies than the BLU and BLA condition. Speech recognition threshold improved from BLU of 65 dB hearing loss and BLA of 48 dB to 26 dB with the Esteem at 12 months. Word recognition scores at 50 dB improved from 10% at BLU and 23% at BLA to 78% with Esteem at 12 months. High frequencies in the speech range, 3,000 and 4,000 Hz, showed a marked improvement. This is a tremendous increase in word recognition.
I was not able to find any reference to the Esteem reducing high-frequency tinnitus. I’m certain this is because tinnitus studies have yet to be conducted on this very new device. I believe, however, that improving high-frequency hearing must have a significant impact on masking tinnitus.
Editor’s Note: Envoy Medical states on their website that the Esteem is contraindicated for “disabling tinnitus.” Individuals with tinnitus who are interested in the Esteem should consult their ENT physician to determine if it is appropriate for them.
There are some significant potential side effects to the procedure. Of the 57 subjects implanted, there were two wound infections. One was resolved medically but the other required removal of the device. There was one delayed facial paralysis, which was resolved with medication. There were also three revisions due to limited benefit.
Currently, the cost of the implant is $30,000. Most insurance companies do not cover it at present though some are beginning to, including some provided by the military.
“I do a lot of work with the military,” said Dr. Seidman. “The number one and number two disabilities for our men and women coming home from Iraq and Afghanistan is hearing loss and tinnitus.”
In years to come, the Envoy Esteem technology and others like it should prove to be of great value to individuals with difficult hearing loss issues.
Refereneces
1 – Kraus EM, Shohet JA, Catalano PJ. Envoy Esteem Totally Implantable Hearing System: phase 2 trial, 1-year hearing results. Otolaryngol Head Neck Surg. 2011 Jul;145(1):100-9.
2 – Shohet JA, Kraus EM, Catalano PJ. Profound High-Frequency Sensorineural Hearing Loss Treatment with a Totally Implantable Hearing System. Otology & Neurotology 32:1428,1431, 2011.
