Why Your Doctor Ordered an MRI for you tinnitus…
By Barry Keate and Mari Quigley Miller
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
Editor’s Note: Mari Quigley Miller developed an acoustic neuroma with hearing loss and tinnitus and has since undergone successful treatment. She now leads a Tinnitus Support Group in Orange, CA. For further information, contact Mari at mariq849 (at) cs.com.
When a person with tinnitus visits their ENT for help, the first steps in diagnosis are typically an audiological examination and an order for an MRI (Magnetic Resonance Imaging). The MRI is performed to rule out the possibility of an acoustic neuroma or other organic cause of the tinnitus.
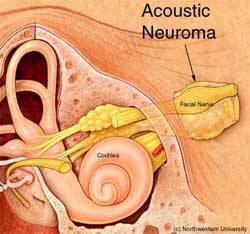 Acoustic neuromas are often referred to by ENTs as Vestibular Schwannomas. They typically arise from the Schwann cells covering the vestibular nerve. They are rare, non-malignant growths that occur on the eighth cranial nerve leading from the brain to the inner ear. They are very slow growing, developing over many years, and are not cancerous. They do not spread but continue growing from the point where they begun.
Acoustic neuromas are often referred to by ENTs as Vestibular Schwannomas. They typically arise from the Schwann cells covering the vestibular nerve. They are rare, non-malignant growths that occur on the eighth cranial nerve leading from the brain to the inner ear. They are very slow growing, developing over many years, and are not cancerous. They do not spread but continue growing from the point where they begun.
The eighth cranial nerve is composed of two parts; one carrying sound and the other carrying balance information to the brain. These lie adjacent to the facial nerve. They pass through a small bony canal called the internal auditory canal that is only 0.8” long. It is in this canal that acoustic neuromas begin. If they grow large enough they will grow out of the internal auditory canal and start to press against the brain. This is where they can become dangerous as they can eventually cause severe pressure on the brainstem and endanger vital functions necessary to sustain life.
Symptoms of acoustic neuroma include gradual hearing loss (primarily on one side only), tinnitus, sometimes dizziness and, in severe cases, facial numbness and tingling. A severe increase in intracranial pressure may result in headaches, clumsy gait and mental confusion. This is a life-threatening complication requiring urgent treatment.
The good news is that acoustic neuromas are very rare. It is estimated that less than one in one hundred thousand people will develop an acoustic neuroma. In patients with unilateral hearing loss and tinnitus, it is believed that only one in one thousand has an acoustic neuroma. However, because of this possibility, patients who present with hearing loss and tinnitus, especially unilateral tinnitus, are often checked to rule out this possibility.
There are three primary treatment options available to patients with an acoustic neuroma:
1 – Observation: Because the tumors are slow growing and are always benign, careful observation over a period of time is appropriate for some patients. Elderly people with relatively small tumors may not be at much risk during their normal life expectancy. Monitoring is performed periodically and if there is no significant growth, observation is continued.
2 – Microsurgery: Surgery may be performed to either partially or totally remove the growth. Permanent hearing loss occurs in a significant portion of people with this condition and partial removal improves the chances of preserving hearing. There is also a possibility of facial paralysis. Facial nerve and hearing are electronically monitored during surgery to limit this occurrence.
3 – Radiation: This technique has been growing in acceptance and reliability. It is non-invasive and can be performed in a one-dose treatment or a multi-dose treatment on an outpatient basis. The principle is that radiation delivered precisely to the tumor will arrest its growth while minimizing injury to surrounding nerves. Facial weakness or numbness occurs in only a small number of patients and is usually temporary. Hearing can be preserved in many cases. Radiosurgery is limited to small or medium tumors; larger ones must be surgically removed.
Michael Seidman, MD, performs many surgeries for acoustic neuroma and is the only surgeon at the Henry Ford Health System who performs them. He offers three different approaches to the surgery depending on the size of the tumor and the patient. The most common form has the disadvantage of guaranteed permanent hearing loss but causes the least amount of facial paralysis. The other two are successful in preserving hearing in up to 75% of people depending on the size of the growth.
Dr. Seidman typically advises against radiation treatment for acoustic neuroma. He usually performs it only on those patients in the elderly population or the extremely ill patient, for whom there is a great risk from surgery. The reasons are that he has seen major strokes, hearing loss, facial paralysis and sometimes continued growth after surgery.
To treat the tinnitus caused by an acoustic neuroma, Dr. Seidman recommends his patients take at least four bottles of Arches Tinnitus Relief Formula® as a first line of attack.
 Mari’s Story
Mari’s Story
Mari Quigley Miller had symptoms of neuroma beginning in 1995. She had tinnitus in one ear which eventually went to both ears. She would feel dizzy and had a slight shooting pain on the left side of her face. The dizziness and pain would come and go but the tinnitus was continuous. Eventually her hearing began to feel muffled and distorted in her left ear. This was the side that turned out to have the growth.
She spent $3,000 of her own money going to doctors, dentists, etc. searching for answers. She finally sought help at the House Ear Clinic in Los Angeles, CA where she met with Dr. William Slattery and his team. She credits Dr. Slattery with saving her life.
She found she had a fast growing acoustic neuroma. It was growing at a millimeter a month, or a little over a centimeter a year. Acoustic neuromas become quite dangerous at 3 cm in size so it was very urgent to remove this growth quickly.
Mari considered radiation therapy but decided she wanted the growth removed from her head, not simply to stop the growth. So she decided to undergo the surgery.
After the surgery she spent 6 days in the hospital then went home to begin recovery. She had to learn to walk again because her balance nerve was cut. She could not hear in her left ear, her left eye would not shut and her tinnitus was very loud.
Two weeks after the surgery, Mari was able to walk on a treadmill. Her balance and facial control improved. She learned other coping techniques that helped her lower her tinnitus. She found she was allergic to wheat gluten and eliminated that from her diet. She got braces on her teeth and addressed TMJ issues. She started eating healthier foods and taking supplements, especially B vitamins. She took a lot of showers so the water sound would mask her tinnitus.
Now, several years later, Mari has tinnitus at a level 1 out of 10. She contacted the American Tinnitus Association and started her own Tinnitus Support Group in Orange County, CA. She has her life back and is very optimistic. She loves sharing her story and helping others with tinnitus. She says helping others to cope with tinnitus helps her appreciate life. She is considering starting another support group for people with acoustic neuroma.
One final word on this subject: This is still considered debatable and is far from settled but some researchers believe cell phones can increase the potential of acoustic neuroma. The Karolinska Institute in Sweden published research in October of 2005 that showed people who used cell phones for 10 years or more had a greater risk of developing acoustic neuroma. Britain’s Health Protection Agency issued a warning that children only switch on cell phones in an emergency. I’m certain there will be more data in the future.
What is an MRI?
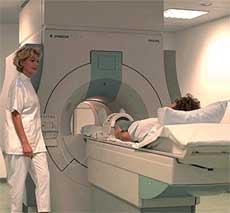 MRI stands for Magnetic Resonance Imaging. This is a method of taking pictures of the tissues in the body without using X-Rays. It was a modern miracle when the first MRI was taken in 1977. For the first time, doctors could look inside a patient’s body without surgery or radiation but by using magnetic waves. The technology has developed to the point that intricately detailed pictures of a small point inside the body can be produced, even in 3-D.
MRI stands for Magnetic Resonance Imaging. This is a method of taking pictures of the tissues in the body without using X-Rays. It was a modern miracle when the first MRI was taken in 1977. For the first time, doctors could look inside a patient’s body without surgery or radiation but by using magnetic waves. The technology has developed to the point that intricately detailed pictures of a small point inside the body can be produced, even in 3-D.
When taking an MRI, the patient is placed on a special table and conveyed inside the machine. The procedure is comfortable and painless but can be very loud. Today’s MRI machines have been described as producing jack hammer-like sounds that can reach 115 dB, a harmful level. Some people are startled by the sound if they have not been forewarned. I have heard many complaints of the noise of an MRI causing a worsening of tinnitus.
 Many imaging centers give patients earplugs or headphones to wear while undergoing the procedure. Others don’t. It is very important for anyone having an MRI to take along foam rubber ear plugs to use if none are offered. The use of earplugs can reduce the decibel level to around 80, which is not harmful and will not exacerbate tinnitus.
Many imaging centers give patients earplugs or headphones to wear while undergoing the procedure. Others don’t. It is very important for anyone having an MRI to take along foam rubber ear plugs to use if none are offered. The use of earplugs can reduce the decibel level to around 80, which is not harmful and will not exacerbate tinnitus.
There is a new generation of MRI scanners entering the market that are considerably quieter than the older ones. A few of these are in imaging centers now but most in use today are the noisy ones. It will take a few years before the new technology becomes widespread and MRIs quiet down.
There are Acoustic Neuroma Support Groups in operation around the US. For more information, visit the Acoustic Neuroma Association at www.anausa.org.
Get Free Shipping!
Order now and get free shipping on either the Tinnitus Starter Kit or Combo Pack. Try the doctor recommended products with clinically proven ingredients for tinnitus. No coupon code required.

