By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
Electrical stimulation of the vagus nerve has been shown to be helpful for chronic depression, controlling intractable epileptic seizures, and now, when coupled with sound therapy, has the potential to reduce noise levels in those with tinnitus.
A new clinical study shows it may be possible in the future to stimulate the vagus nerve externally, bypassing expensive and invasive surgery.
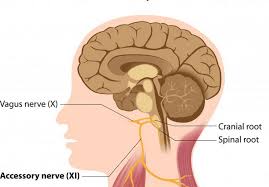 The vagus nerve is the longest of 12 paired cranial nerves. It extends from the base of the brain and connects through the neck, chest and down to the abdomen. There are a number of branching nerves that come in contact with the heart, lungs, larynx, stomach and ears.
The vagus nerve is the longest of 12 paired cranial nerves. It extends from the base of the brain and connects through the neck, chest and down to the abdomen. There are a number of branching nerves that come in contact with the heart, lungs, larynx, stomach and ears.
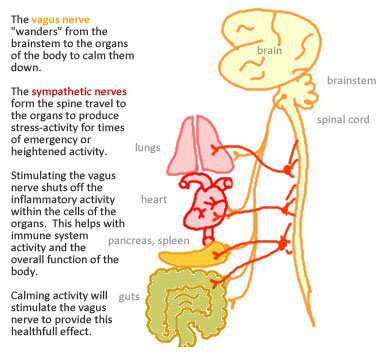
The cranial nerves reside mostly in the head region and control much of what goes on in the face and neck. But the vagus nerve, also known as the tenth cranial nerve, influences the body and brain more than most. It is responsible for speech, swallowing, keeping the larynx open for breathing, slowing heart rate, reducing blood pressure, initiating digestive processes and modulating inflammation.
Besides output to the various organs in the body, the vagus nerve conveys sensory information about the state of the body’s organs to the central nervous system. Eighty to ninety percent of the nerve fibers in the vagus nerve are sensory nerves communicating the state of the body and digestion to the brain.
Vagus Nerve Stimulation (VNS)
Stimulating the vagus nerve through electrical impulses causes the release of neurotransmitters and elevated levels of the inhibitory neurotransmitter GABA, which reduces heart rate, controls epileptic seizures and alters mood patterns. It has the ability to train the brain to reorganize and reassign neurons to the locations where they are most needed.
For instance, when someone is exposed to a stressful event, a hormone called epinephrine is released into the bloodstream, which activates the vagus nerve. The nerve then sends a signal to the brain to release the neurotransmitter norepinephrine, which assigns extra neurons and strengthens memory storage for emotional feelings of that specific time. This is why people often vividly remember traumatic events in specific detail. The vagus nerve is sending a signal telling the brain what to learn and when to learn it. (1) The reassigning of neurons is called brain plasticity and demonstrates that the brain has the ability to rewire itself.
Because the vagus nerve is associated with many different functions and brain regions, research is being done to determine its usefulness in treating other illnesses, including various
anxiety disorders, Alzheimer’s disease, Parkinson’s disease, migraines, fibromyalgia, and, as we shall soon investigate, tinnitus. (2)
VNS is a one treatment in a group of therapies called electrical stimulation. Therapies of this type include cochlear implantation, Transcranial Magnetic Stimulation and direct stimulation by means of implanted electrodes.
VNS in Laboratory Rats
Researchers from the University of Texas – Dallas were interested in pairing VNS with a specific movement to see if the brain reorganization in laboratory rats would affect the ability to perform the movement. (3) The team analyzed the brain activity in response to the stimulation after 5 days of stimulation and movement pairing. They found the rats that received the stimulation and the movement training displayed large changes in the organization of the brain’s movement control system. Those rats that received identical movement training without paired stimulation did not experience any brain changes, or plasticity.
People who suffer brain trauma or strokes generally undergo rehabilitation that involves repeated movement of the affected limb in an effort to regain motor skills. Frequent use of the affected limb leads to reorganization in the brain that is vital to recovery.
This research indicates that paring standard therapy with VNS may result in a faster and more extensive brain reorganization and may speed up recovery.
Investigators at UT Dallas also investigated the ability of VNS to stimulate cortical reorganization to restore neuronal activity to normal and reverse tinnitus in laboratory rats. (4)
“When we paired tones with brief pulses of VNS we eliminated the physiological and behavioral symptoms of tinnitus in noise-exposed rats,” said the lead author Navzer D. Engineer, PhD. The animals were monitored for three weeks after the therapy and the changes remained constant. “Pairing sounds with VNS provides that precision by rewiring damaged circuits and reverses the abnormal activity that generates the phantom sound.”
In answering a question about VNS for tinnitus (Ask Barry/March 2011) a reader asked, “How can one tell that tinnitus is improved in rats? There is not an audiological device in the world that can measure and quantify tinnitus without the subject being able to communicate with the doctor, and rats can’t speak!” This led to the writing of a previous article on An Animal Model of Tinnitus.
The theory behind VNS for tinnitus is as follows: When one neuron sends a signal to another neuron in the brain, it is typically referred to as a ‘spike’. When we hear sound, cells in the brain’s auditory cortex generate a large number of spikes in complex patterns. In the absence of sound, the brain has a low level of this spiking activity. In the tinnitus brain, however, the neurons at the tinnitus frequency are highly excitable. Hundreds of thousands of nearby neurons fire simultaneously in the tinnitus frequency whether there is outside stimulus or not. This simultaneous firing of brain cells is referred to as synchrony, which is thought to be one of the mechanisms responsible for sounds perceived by tinnitus patients. (1)
By consistently pairing VNS with all other tones except the tinnitus tone, the other neuron groups expand and the tinnitus tone neurons shrink. Over time the brain learns to ignore the tinnitus tone. Pairing several of these tones (except the tinnitus tone) helped subdue the abnormal hyperactivity and restored the auditory cortex activity back to normal in a rat model of tinnitus.
VNS in Humans
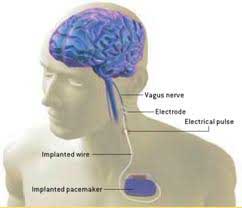
Previously, VNS therapy in humans has required the implantation of a device much like a pacemaker, about the size of a stopwatch, along with a battery pack to power it. In recent years developments in microelectronics and microtransponders allow for the implantation of tiny semiconductor devices no bigger than a grain of salt to the sites of stimulation. Activation of the devices depends on external sources using radio waves or near infrared light.
Dr. Navzer Engineer, lead researcher at UT Dallas, is also developing this technology as Vice President of Preclinical Affairs at MicroTransponder, a medical device company and spin-off of UT Dallas.
Recently, MicroTransponder performed a 10-patient clinical study to evaluate the safety and preliminary effectiveness of Paired VNS Tone Therapy in humans. (5) The study was conducted at University Hospital, Antwerp in Belgium under the supervision of Dirk De Ridder, MD, PhD., and his team.
Therapy sessions lasted two and a half hours daily for a month. During the study, patients sat in a comfortable chair and wore headphones, listening to tones while receiving small bursts of neurostimulation, which activated the vagus nerve.
Assessments were made using standard tinnitus questionnaires and a measure called minimum masking level (MML). The MML indicates how loud a sound must be to mask a person’s tinnitus. Average MML improvement was 11 dB and six of the patients had an average of 22 dB improvement. Several patients reported their tinnitus improved after one month of treatment. Improvement lasted for two months up to a year. It is important to note that not all patients had an improvement.
A recent government grant allowed MicroTransponder to begin a US clinical trial that will involve 30 patients.
Discussion
While the promise of VNS for tinnitus is great, there is a lot of work to be accomplished before it can become a widespread, effective therapy. In the case of cochlear implants, it was 10 years after the original devices were first introduced before they were refined enough that they became implantable.
There are significant, though not life-threatening, side effects of the therapy, which has been used on about 50,000 people for severe epilepsy and treatment resistant depression. (2) Sleep apnea has been consistently demonstrated in patients with VNS implants of which a minority report severe obstructive sleep apnea. The obstructive events can be controlled by decreasing the frequency or intensity of the stimulation or by having the patient sleep in a partial sitting position.
Other side effects include alteration of voice (66%), coughing (45%), inflammation of the throat (35%), and throat pain (28%). Hoarseness is very common. Other symptoms may include headache, nausea, vomiting and indigestion.
Surgery or implantation of any kind should only be considered after less invasive means have been exhausted. It is also important to note that VNS, while FDA approved for treating depression and seizures, is not FDA approved for treating tinnitus and remains in clinical trials. Regular cost for the implantation procedure alone is $20,000.
Recently, a clinical study has shown that the Vagus nerve can be reached and stimulated at a location in the outer ear, the cymba conchae. (6)
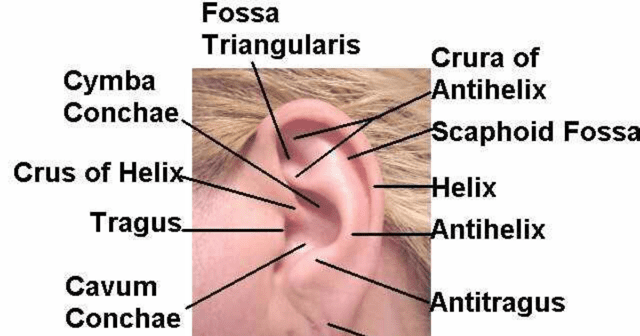
Researchers had previously shown in studies in laboratory animals that the auricular branch of the vagus nerve could be stimulated through the outer ear. This study, conducted on humans, used electrical stimulation to the earlobe on control subjects and active stimulation to the cymba conchae on active subjects. It clearly showed that stimulating the cymba cochlea produced activation of the central vagus nerve while stimulating the ear lobe did not.
These findings provide evidence that the projections of the vagus nerve are linked to the central vagus nerve and can be accessed non-invasively via the external ear. Future research will determine parameters for the fine tuning of stimulation; pulse width, frequency and electrical intensity.
References:
1 – Rosellini W, Gurnes J, Engineer N. Vagus Nerve Stimulation: New Potential for Tinnitus Relief. Tinnitus Today Summer, 2012.
2 – http://en/wikipedia.org/wiki/Vagus_nerve_stimulation
3 – Porter BA, Khodaparast N, Fayyaz T, et al. Repeatedly Pairing Vagus Nerve Stimulation with a Movement Reorganizes Primary Motor Cortex. Cereb Cortex. 2012 Oct:22(10):2365-74.
4 – Jamie T. Vagus Nerve Stimulation Helps resolve Tinnitus in Rats–Clinical Trials to Follow. Neurology Today. 17 February 2011–Volume 11–Issue 4 – pp 1, 12-14.
5 – Press Release 7/15/12; http://wwwmicrotransponder.com/?page_id=233
6 – Frangos E, Ellrich J, Komisurak BR. Non-invasive Access to the Vagus Nerve Central Projections via Electrical Stimulation of the External Ear: fMRI Evidence in Humans. Brain Stimul 2015 May-June;8(3):624-36.
