By Barry Keate
Barry Keate, has lived with tinnitus over 40 years and has published 150+ research articles on numerous aspects of tinnitus. He is an expert on the condition and a well-known advocate for those with tinnitus.
The most common cause of tinnitus is exposure to noise, with approximately 70% of people with tinnitus having noise-induced hearing loss. Somewhat surprisingly, the second most common cause of tinnitus is head and neck injuries. In a clinical study of 2,400 tinnitus patients at the Oregon Health Science University, more than 12% reported that their tinnitus had been caused by head or neck injury. (1)
There are two broad categories of head and neck injury, Traumatic Brain Injury (TBI) and whiplash. Two other, somewhat rare conditions are part of the complex of head and neck injuries. These are instability of the craniocervical junction at the top of the spine and Chiari Malformation, a congenital defect in the base of the skull.
Traumatic Brain Injury (TBI)
TBI occurs when a sudden trauma or head injury disrupts the function of the brain. TBI is often called the signature wound of the Iraq and Afghanistan wars. A common cause of TBI in these conflicts is the detonation of Improvised Explosive Devices (IEDs) targeting American troops. TBI can also be caused by automobile accidents and sports injuries, especially in football.
The Centers for Disease Control estimates that 1.7 million Americans suffer from TBI every year and that 5.3 million Americans are now living with brain injuries. (2)
Brain injuries are classified as mild, moderate and severe. The mild form is usually referred to as a concussion. This is what happened recently to Hillary Clinton, the US Secretary of State, who became dehydrated due to a virus. She then became dizzy and fell in her home. She suffered a concussion and was taken to the hospital for several days.
Some symptoms of mild TBI can be evident immediately while others may not surface for several days or even weeks after the injury. A person with mild TBI may remain conscious or may experience a loss of consciousness for a short period. The person may feel dazed for several days or weeks. Other symptoms include headache, confusion, lightheadedness, dizziness, blurred vision, hearing loss with tinnitus, behavioral or mood changes, and trouble with memory, concentration, attention or thinking.
One clinical study found that after minor head trauma, most patients suffer from dizziness and more than half complain of tinnitus and hearing loss. (3)
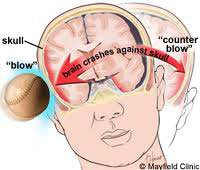
A person with moderate or severe TBI may show the same symptoms but may also have a headache that gets worse or does not go away, repeated vomiting or nausea, convulsions or seizures, inability to awaken from sleep, dilation of one or both pupils, slurred speech and loss of coordination. (4)
As mentioned above, concussion is the most minor and most common type of TBI. More serious injuries may involve skull fractures, which can cause bruising of brain tissue called a contusion. Damage to a major blood vessel in the head can cause a hematoma, or heavy bleeding into or around the brain.
Another insult to the brain that can cause damage is anoxia. This is a condition where there is an absence of oxygen supply to the tissues. Without oxygen, cells in the brain die within several minutes.
Little can be done to reverse the initial brain damage caused by trauma so medical personnel try to stabilize the patient and focus on preventing further injury. Primary concerns include insuring proper oxygen supply to the brain and the rest of the body, maintaining adequate blood flow and controlling blood pressure.
Because many head-injured patients may also have spinal cord injuries, medical personnel take great care in moving the patient. The patient is usually placed on a backboard and in a neck restraint. These devices immobilize the patient and prevent further injury to the head and neck.
Patients with mild to moderate injuries may receive skull and neck X-rays to check for bone fractures or spinal instability. More severely injured patients may receive a CT scan which can show bone fractures as well as the presence of hemorrhage, hematomas, contusions, brain tissue swelling and tumors.
Sometimes during TBI swelling occurs and fluids accumulate within the brain space. This increases pressure on the brain and is called intracranialpressure (ICP). If a patient has high ICP, he or she may undergo a ventriculostomy, a procedure that drains cerebrospinal fluid from the brain to bring the pressure down.
After brain trauma large amounts of neuronal damage can occur. The neuron is the main functional cell of the brain and nervous system, consisting of a cell body (soma), a tail or long nerve fiber (axon), and projections of the cell body called dendrites. The axons travel in tracts or clusters throughout the brain, providing extensive interconnections between brain areas.
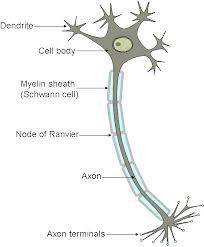
One of the most pervasive types of injury following even minor trauma is damage to the nerve cell’s axon through shearing. This is referred to as diffuse (widespread) axonal injury. This damage causes swelling of the axon and disconnection from the neuron. Additionally, the neuron degenerates and releases toxic levels of the excitatory neurotransmitter glutamate. This damages neighboring neurons that were not initially harmed during the injury and causes them to initiate programmed cell death, or apoptosis. This process usually takes place within the first 24 to 48 hours.
In the healthy brain, the chemical glutamate functions as a neurotransmitter, but an excess of glutamate causes neurons to quickly overload from too much excitation, releasing toxic chemicals. These chemicals poison the environment of surrounding cells, initiating degeneration and programmed cell death. (5)
The brain attempts to repair itself after a trauma and is somewhat successful in cases of mild TBI. Neurons can recover by sprouting some of the remaining healthy fibers into the spaces once occupied by the degenerated axon. These fibers can help the neuron resume communication with neighboring neurons. However, the process is very delicate and can be disrupted by neuroexcitation, caused by glutamate. This excitation disrupts the natural recovery process and can cause sprouting fibers to lose direction and connect with the wrong terminals.
Scientists suspect that these misconnections may contribute to some long-term disabilities such as pain, spasticity, seizures and memory problems.
We have discussed the role of glutamate in neurodegenerative conditions many times in the past. It is thought to be the primary villain in causing tinnitus, Parkinson’s disease, multiple sclerosis, epilepsy, and more.
Arches Tinnitus Formula (ATF) may be of help in reducing neuronal death in TBI patients. Ginkgo biloba, the primary ingredient in ATF is known to be a glutamate antagonist and neuroprotector.
A review of clinical studies conducted at the Center for Research in Complementary and Alternative Medicine found Ginkgo shows promise in treating some of the Neurological problems associated with TBI. (6)
Ginkgo biloba should not be given to anyone who may have bleeding problems due to TBI. It can potentially thin the blood and aggravate the bleeding. It should only be used after physicians have determined there is no bleeding.
For more information on the subject read Part 2 of Head and Neck Injuries Cause Tinnitus which discusses whiplash and other causes.
References:
1 – Folmer RL, Griest SE. Chronic tinnitus resulting from head or neck injuries. Laryngoscope 2003 May;113(5):821-7.
2 – http://www.cdc.gov/traumaticbraininjury/
3 – Kisilevski V, Podoshin L, et al. Results of Otovestibular Test in Mild Head Injuries. International Tinnitus Journal, Vol. 7 No 2 – July / Dec, 2001
4 – National Institute of Neurological Disorders and Stroke. Traumatic Brain Injury: Hope Through Research. http://www.ninds.nih.gov/disorders/tbi/detail_tbi.htm
5 – ibid.
6 – Diamond BJ, Shiflett SC, Feiwei N, et al. Ginkgo biloba etract: Mechanism and clinical indications. Archives of Physical Medicine and Rehabilitation, Volume 81, Issue 5, pp 668-678, May, 2000.
Get Free Shipping!
Order now and get free shipping on either the Tinnitus Starter Kit or Combo Pack. Try the doctor recommended products with clinically proven ingredients for tinnitus. No coupon code required.

